The way multiple sclerosis (MS) is diagnosed is undergoing a major transformation. An international panel of experts has updated the McDonald Diagnostic Criteria—the gold standard used by neurologists worldwide. Published in The Lancet Neurology, the revisions promise to make diagnosis faster, more accurate, and more accessible for patients of all ages. For thousands living with MS, this shift could mean earlier treatment, better long-term outcomes, and reduced uncertainty during the most critical stage of the disease.
For decades, MS diagnosis was a prolonged process, often leaving patients waiting years for confirmation. By contrast, the latest update aims to reduce the diagnostic window from months to potentially just weeks. Timothy Coetzee, President and CEO of the National MS Society, describes the progress as a “turning point” for clinical practice: “Decades ago, it could take years to diagnose MS. Today it is down to months. And soon, we expect it to get even easier and faster.”
What the New Criteria Change
The McDonald criteria, first introduced in 2001, have been revised several times to reflect advances in medical imaging, research, and clinical experience. The last major update in 2017 already shortened the average time to diagnosis from four years to about one year. The 2024 revision goes further.
Key updates include:
- Broader patient scope: Clearer considerations for children and adults over 50, who often present with atypical or overlapping symptoms.
- Accessible tools: Integration of diagnostic methods that are less invasive, more affordable, and widely available, reducing reliance on costly or complex imaging alone.
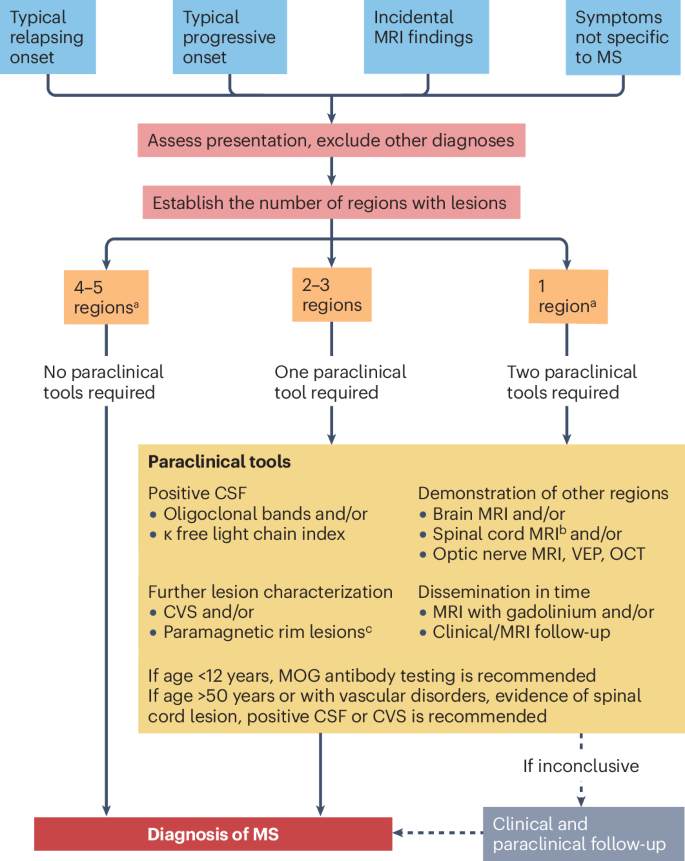
- Evidence flexibility: Expanded criteria for demonstrating “dissemination in time and space”—a cornerstone in diagnosing MS—using new combinations of clinical signs and laboratory data.
This effort was led by the International Advisory Committee on Clinical Trials in Multiple Sclerosis, in collaboration with clinicians, researchers, and advocacy organizations. The revisions reflect a growing recognition that faster diagnosis is not just a medical priority but also a matter of patient well-being.
Why Early Diagnosis Matters
MS is an autoimmune disorder in which the body’s immune system mistakenly attacks the protective coverings of nerve fibers. The result is nerve damage that disrupts communication between the brain and the rest of the body. Symptoms range widely—from fatigue and blurred vision to mobility issues and cognitive decline—making diagnosis notoriously complex.
The earlier patients begin treatment, the more effectively the disease course can be altered. According to neurologists, timely initiation of disease-modifying therapies (DMTs) can reduce relapses, slow disability progression, and preserve brain tissue. Without treatment, patients experience faster brain atrophy compared to healthy individuals of the same age.
As Mariana Marcín, Neurologist at ABC Medical Center, explains: “Treatment of MS has three pillars: managing acute relapses, modifying the disease course, and addressing ongoing symptoms. When treatment starts early, each of these becomes more effective, ultimately protecting independence and quality of life.”
Mexico’s MS Landscape
In Mexico, more than 20,000 people live with MS, and prevalence is highest among women aged 20 to 40. This makes MS the second leading cause of disability in young adults, according to Irene Treviño, Academic at the Faculty of Medicine, UNAM. The impact is not only personal but also social and economic, as disability during prime working years affects families and communities.
“Unfortunately, MS is common, and early intervention significantly influences its progression,” says Jhali Hernández, Co-Founder of Otium Physiotherapy and Wellness. Her remarks highlight a central challenge in Latin America: while diagnostic tools and therapies exist, barriers such as cost, limited specialist availability, and uneven healthcare infrastructure delay access.
The updated McDonald criteria could help bridge this gap by introducing diagnostic pathways that rely less on advanced imaging and more on clinical evidence and widely available tests.
Treatment Approaches and Long-Term Management
Managing MS is not limited to diagnosis—it is a lifelong process. Current treatment strategies include:
- Acute relapse management: High-dose corticosteroids, such as methylprednisolone, to quickly reduce inflammation and restore function.
- Disease-modifying therapies (DMTs): Medications that alter the disease trajectory, reducing relapses and slowing disability progression. Over 20 DMTs are now approved globally, ranging from injectables to oral drugs and infusions.
- Symptom management: Tailored interventions for fatigue, spasticity, mobility, and cognitive symptoms. This often involves a combination of medication, physiotherapy, and lifestyle adjustments.
Despite these advances, MS remains a progressive disease. Brain atrophy and worsening disability continue in many patients, albeit at a slower pace with treatment. This reality underscores the importance of innovation in both diagnostics and therapies.
The Global Push for Accessible MS Care
The revision of diagnostic criteria is part of a broader international movement to improve MS outcomes. Organizations like the National MS Society, ECTRIMS (European Committee for Treatment and Research in MS), and regional advocacy groups have consistently pushed for earlier, more equitable access to care.
The emphasis on affordability and accessibility in the new guidelines is particularly important for low- and middle-income countries. By widening the diagnostic toolbox, the revisions reduce reliance on expensive MRI scans, which are not always available in rural or under-resourced healthcare systems.
Global collaboration is a recurring theme. The updates represent the input of hundreds of experts across continents, reflecting diverse healthcare realities. As Coetzee puts it, “This is about equipping healthcare professionals everywhere with the tools to make earlier and more accurate diagnoses, regardless of geography.”
What This Means for Patients
For those already diagnosed, the criteria changes will not alter their clinical management. However, for individuals currently undergoing evaluation—or those experiencing unexplained neurological symptoms—the path to answers may become shorter and clearer.
Faster diagnosis means:
- Reduced uncertainty and psychological stress for patients and families.
- Earlier access to therapies that can slow disease progression.
- Better planning for lifestyle adjustments, financial security, and family responsibilities.
- Greater potential to maintain long-term independence.
For healthcare systems, shorter diagnostic delays translate into lower long-term costs, as early treatment reduces the need for expensive hospitalizations and disability support.
Looking Ahead
MS research is advancing rapidly, with new biomarkers, imaging technologies, and artificial intelligence tools on the horizon. The updated McDonald criteria are a step forward but also a foundation for future refinement. Experts anticipate further integration of blood tests, genetic data, and advanced imaging into routine practice within the next decade.
In Mexico and beyond, the challenge now lies in implementation. Training clinicians, updating protocols, and ensuring equitable access to diagnostic tools will be critical. Advocacy groups stress that guidelines only have impact if healthcare providers can apply them consistently.
The message is clear: MS is no longer a disease defined by years of diagnostic uncertainty. With updated criteria, global collaboration, and a focus on accessibility, the future of MS care is shifting toward earlier intervention, more personalized treatment, and better patient outcomes.
This development is not just a scientific update—it is a tangible improvement in how patients experience one of the most life-altering neurological conditions. For the 20,000 Mexicans living with MS, and the millions worldwide, the revised guidelines mark a critical step toward faster answers, stronger treatment, and hope for a more manageable future.